Facet Joint Injury and Whiplash
From a clinical and medical-legal perspective, clinical instability is quite important. Clinical instability implies substantial injury, poor recovery, impairment and disability. One study notes that up to 30% of those with clinical instability “may suffer permanent neurologic sequelae (1).”
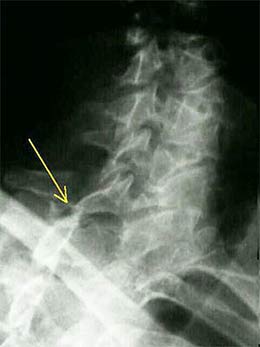
The primary motor vehicle collision injury is to the facet joint capsules (2), and facet injury alone can cause clinical instability (5). However, it is established that the injury can extend to involve the intervertebral disc (3), and also the anterior longitudinal ligament (4). Injuries to the intervertebral disc and anterior longitudinal ligament are more serious than facet capsular injuries, and are much more likely to result in clinical instability.
There has been much controversy over the injury mechanism that occurs in rear-end auto collisions. Some of the insurance companies have either tried to deny that anyone gets injured at all or have attributed the injury to strained muscles. However, recent research by Barnsley et al indicates that the source of the pain in a majority (~60%) of whiplash patients is the zygapophyseal (facet) joints, rather than the muscles. (5,6)
The most common levels of zygapophyseal joint pain found in this study were at the C2/3 and C5/6 levels. These researchers used sophisticated injections of anesthetics into the facet joints under fluoroscopic guidance to determine this, though, and such injury to the soft tissue structures of the zygapophyseal joints (such as the joint capsules) are not easily seen with x-ray, CAT scans or MRI. But if needed, facet blocks could be done by anesthesiologists to prove these injuries in a medico-legal environment.
We know that many people in low speed collisions are injured and that a large number of these patients continue to report symptomatology for years after their accidents.(7,8) These patients continue to have pain long after their cases are settled, thus dispelling the myth that we are dealing with “litigation neurosis.”(9,10) Barnsley, et al. reviewed the studies that have followed up on whiplash patients for a period of time after the injury and have come up with a conservative estimate of between 14 to 42% of whiplash patients who develop chronic neck pain and 10% who will have constant, severe pain indefinitely. (11)
A new study by Kaneoka et al (12) now provides a demonstration of the mechanism of the whiplash injury and how the zygapophyseal joints and other spinal structures are injured. Kaneoka used cineradiography of human volunteers while undergoing a simulated rear end collision and found an unusual pattern of movement of the cervical vertebrae. The lower cervical segments rotate around an abnormally high instantaneous axis of rotation. In particular, C6 starts to extend before the rest of the spine. This results in an s-shaped configuration of the spine as C6 extends and the rest of the spine initially flexes. Then, as the rest of the cervical spine extends, this results in an extreme rotational torque at the C5/6 level. This results in a stretching of the anterior longitudinal ligament and forces the inferior facet of C5 to collide with the superior facet of C6. This may result in impingement and inflammation of the folds of synovial tissue between the zygapophyseal joints (facet synovial fold impingement syndrome). And Giles has previously demonstrated that these synovial folds are pain sensitive.(13)
In conclusion, we now have evidence that the anatomical structures most commonly injured in low speed whiplash injuries are the zygapophyseal (facet) joints and we have a mechanism to explain how this injury occurs. And such a joint injury cannot always be expected to heal within 6 weeks and could explain why some whiplash patients continue to experience pain for long periods of time after their accidents and why they have a higher incidence of degenerative spinal changes in the cervical spine years later. Also, since chiropractors can specifically treat the zygapophyseal joints with specific manipulative techniques, we may be the most qualified professionals to treat these injuries. In fact, several researchers have hypothesized that one of the most important benefits of manipulation is freeing up entrapped folds of synovial tissue between the zygapophyseal joints.(13,14)
Ligaments and disc
Magnetic resonance and autopsy studies of whiplash patients have documented injuries to the neck ligaments and intervertebral discs in addition to the facet joints. Ligament injuries may cause acute neck pain and lead to chronic spinal instability, abnormal muscle response patterns and decreased neck mobility.
Ligaments of the upper cervical spine have unique functional and structural anatomy, predisposing them to partial or complete rupture at low strains. Ligaments provide joint position sense during normal motion and combined with discs provide stability and absorb energy during high speed trauma. The specific function of each cervical ligament and disc in resisting whiplash loading is dependent upon its specific anatomical location, orientation, geometry, and unique mechanical properties.
Spinal ligaments and fibers encapsulating the discs can partially or completely rupture when stretched beyond their physiological limit. The whiplash related response of the cervical ligaments and discs of the neck have been quantified using a whole cadaveric cervical spine model with muscle force replication. During rear impacts with the head facing forward, dynamic strains in the anterior longitudinal ligament and annular disc fibers above physiological levels and increased joint laxity were observed. The C5/C6 disc was found to be at highest risk of injury. The disc injuries occurred at lower impact accelerations during rear impacts compared to frontal impacts.
Ligament damage may cause instability resulting in loss of motion segment integrity which can be evaluated with flexion/extension x-rays. The AMA Guides to the Evaluation of Permanent Impairment, 5th edition, Nov. 2000, Chapter 15, pages 378-392 place a high impairment rating on loss of motion segment integrity, equating this damage as equal to a vertebra that has a compression fracture greater than 50%. This ligament instability often interferes with normal neck posture, altering the structure of the cervical spine which may lead to chronic health problems.
Damage to the disc in whiplash injuries may cause an early onset of degenerative disc disease. An article published in Injury. 1991 Jul;22(4):307-9, indicated a significantly higher rate of disc degeneration was found in whiplash patients 10 years after the accident when compared to age matched controls.
It should be noted that a normal MRI study of the neck does not exclude the existence of clinically significant disc disease in whiplash patients suffering chronic neck, head or nerve pain. Internal Disc Disruption is a condition where the internal structure of the disc is disrupted, while the external appearance is essentially unchanged.
The cascade events to facet joints following whiplash:

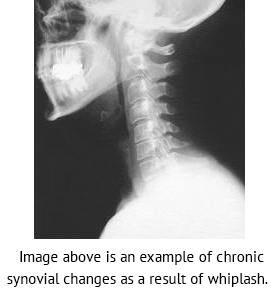
The most recent comprehensive review of the Synovial Fold Entrapment Syndrome is written by Alexandra Webb and colleagues and will be published in the April 2011 issue of the journal Manual Therapy (Epub at this time, 2/15/11) (11).
In this article, Dr. Webb and colleagues note that intra-articular synovial folds are formed by folds of synovial membrane that project into the joint cavity. Cervical spine synovial folds extend 1–5 mm between the articular surfaces. Synovial folds are found in synovial articulations throughout the vertebral column. Synovial folds in the vertebral column were first documented in 1855.
Dr. Webb and colleagues note that the published literature uses a number of names to identify these synovial folds, including:
- “Synovial fold is the most accurate name to apply to these structures.”
- Meniscus / Menisci
- Meniscoid
- Intra-articular inclusions
- Intra-articular discs
Anatomically, synovial folds contain an abundant vascular network and sensory nerve fibers (11).
The entrapment hypothesis is usually proposed to explain the clinical presentations of the synovial fold syndrome. “An abnormal joint movement may cause a synovial fold to move from its normal position at the articular margins to become imprisoned between the articular cartilage surfaces causing pain and articular hypomobility accompanied by reflex muscle spasm (11).”
“Synovial fold entrapment has been used to explain the pathophysiology of torticollis and the relief of pain and disability following spinal manipulation.” The traction forces generated during manipulation would cause release of a trapped fibro-adipose synovial fold from between the articular surfaces (11).
Additionally, contusions, rupture and displacement of the synovial folds have been reported at autopsy following fatal motor vehicle trauma; these injuries are not visible at post-mortem using conventional X-ray, CT or MRI (11).
With repeated mechanical impingement between the articular surfaces, the synovial fold may differentiate into fibrous tissue to varying degrees. The fibrous apex of the synovial indents the articular hyaline cartilage, further entrapping the apex of the synovial fold. Manipulative therapy may traction and separate the articular surfaces apart, releasing the entrapped synovial fold. (Drawing below based on #1).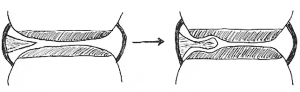 Historically, the entrapped synovial fold syndrome has been written about for decades. In the 1971 translation of their authoritative reference text The Human Spine in Health and Disease, Drs. Schmorl and Junghanns note (12):
Historically, the entrapped synovial fold syndrome has been written about for decades. In the 1971 translation of their authoritative reference text The Human Spine in Health and Disease, Drs. Schmorl and Junghanns note (12):
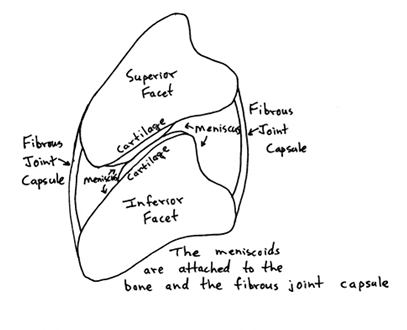
“Like other body articulations, the apophyseal joints are endowed with articular capsules, reinforcing ligaments and menisci-like internal articular discs.”
“Like any other joint, the motor segment may become locked. This is usually associated with pain.” Chiropractors refer to such events as subluxations. These motor unit disturbances can cause torticollis and lumbago.
“Various processes may cause such ‘vertebral locking.’ It may happen during normal movement. The incarceration of an articular villus or of a meniscus in an apophyseal joint may produce locking.”
If a joint is suddenly incarcerated within the range of its physiologic mobility, as occurs with the meniscus incarceration of the knee joint, it is an “articular locking or a fixed articular block.”
“Such articular locking is also possible in the spinal articulations (apophyseal joints, intervertebral discs, skull articulations, lumbosacral articulations). They may be mobilized again by specific therapeutic methods (stretchings, repositioning, exercises, etc.). Despite many opinions to the contrary, this type of locking is today increasingly recognized by physicians. Many physicians are employing manipulations which during the past decades were the tools of lay therapists only (chiropractors, osteopaths). However, these methods have at times been recommended by physicians. They have also been known in folk medicine and in medical schools of antiquity.”
Schmorl and Junghanns’ text includes two photographs of anatomical sections through the facet joints showing these “menisci-like internal articular discs,” or meniscus. They also included three radiographs and one drawing showing abnormal gapping of an articulation as a consequence of meniscus entrapment in a facetal articulation. They note that such a meniscoid incarceration can cause acute torticollis, and they show a “follow-up roentgenogram after manual repositioning” resulting in “immediate relief of complaints and complete mobility.”
In 1985, 30 distinguished international multidisciplinary experts collaborated on a text titled Aspects of Manipulative Therapy (13). The comments in this text pertaining to the interarticular meniscus (synovial entrapment syndrome) include:
“Histologically, meniscoids are synovial tissue.”
“Their innervation is derived from that of the capsule.”
The current hypothetical model of the mechanism involved in acute joint locking is based on a phenomenon in which the “meniscoid embeds itself, thereby impeding mobility.”
“It is highly probable that the meniscoids do play an important role in acute joint locking, and this is confirmed by the observation that all the joints afflicted by this condition are equipped with such structures.”
In 1986, physical therapist Gregory Grieve authored a text titled Modern Manual Therapy of the Vertebral Column (14). This text boasts 61 international multidisciplinary contributors, contains 85 topic chapters, and is 898 pages in length. In the chapter titled “Acute Locking of the Cervical Spine” the text notes that a cause of acute cervical joint locking includes:
“Postulated mechanical derangements of the apophyseal joint include nipped or trapped synovial fringes, villi or meniscoids.”
In her 1994 text Physical Therapy of the Cervical and Thoracic Spine, professor of physiotherapy from the University of South Australia, Ruth Grant writes (15):
“Acute locking can occur at any intervertebral level, but is most frequent at C2-C3. Classically, locking follows an unguarded movement of the neck, with instant pain over the articular pillar and an antalgic posture of lateral flexion to the opposite side and slight flexion, which the patient is unable to correct. Locking is more frequent in children and young adults. In many, the joint pain settles within 24 hours without requiring treatment (because the joint was merely sprained or because it unlocked spontaneously), but other patients will require a localized manipulation to unlock the joint.”
In his 2004 text titled The Illustrated Guide to Functional Anatomy of the Musculoskeletal System (16), renowned physician and author Rene Cailliet, MD comments on the anatomy of the interarticular meniscus, stating:
“The uneven surfaces between the zygapophyseal processes are filled by an infolding of the joint capsule, which is filled with connective tissue and fat called meniscoids. These meniscoids are highly vascular and well innervated.”
In the fourth edition of his textbook Clinical Anatomy of the Lumbar Spine and Sacrum (7), physician, anatomist, and researcher Dr. Nikolai Bogduk writes:
“The largest of the meniscoid structures are the fibro-adipose meniscoids. These project from the inner surface of the superior and inferior capsules. They consist of a leaf-like fold of synovium which encloses fat, collagen and some blood vessels.”
“Fibro-adipose meniscoids are long and project up to 5 mm into the joint cavity.”
“A relatively common clinical syndrome is ‘acute locked back.’ In this condition, the patient, having bent forward, is unable to straighten because of severe focal pain on attempted extension.”
“Maintaining flexion is comfortable for the patient because that movement disengages the meniscoid. Treatment by manipulation becomes logical.”
The January 15, 2007 publication of the top ranked orthopaedic journal Spine contains an article titled (18):
High-Field Magnetic Resonance Imaging of Meniscoids
in the Zygapophyseal Joints of the Human Cervical Spine
Key Points From this article include:
- Pain originating from the cervical spine is a frequent condition.
- Neck pain can be caused by pathologic conditions of meniscoids within the zygapophysial joints.
- “Cervical zygapophysial joints are well documented as a possible source of neck pain, and it has been hypothesized that pathologic conditions related to so called meniscoids within the zygapophysial joints may lead to pain.”
- The meniscoids of the cervical facet joints contain nociceptors and may be a source of cervical facet joint pain.
- Proton density weighted MRI image sequence is best for the evaluation of the meniscoid anatomy and pathology.
- Meniscoids are best visualized with high-field MRI of 3.0 T strength.
- Meniscoids are best depicted in a sagittal slice orientation.
- The meniscoids in C1-C2 differ from those in the rest of the cervical spine.
- Meniscoids may become entrapped between the articular cartilages of the facet joints. This causes pain, spasm, reduced movement, and “an acute locked neck syndrome.” “Spinal adjusting can solve the problem by separating the apposed articular cartilages and releasing the trapped apex.”
 Clinical Applications
Clinical Applications
Decades of evidence support the perspective that the inner aspect of the facet capsules have a process that extends into and between the facet articular surfaces. This evidence includes anatomical sections, histological sections, MR imaging, and clinical evaluations. This synovial fold can become entrapped between the facet articulating surfaces, producing pain, spasm, and antalgia. Published terminology for the anatomy includes synovial fold, synovial villus, meniscoid, meniscoid block, and joint locking.
Using the cervical spine as a representative model, a classic clinical presentation would be that of an acute torticollis. If the synovial fold is entrapped on the left side of the cervical spine, the patient would present with an antalgia of right lateral flexion; in other words, the patient bends away from the side of entrapment. The patient’s primary pain symptoms will be on the side of entrapment, in this example, the left side. Active range of motion examination will show that the patient is capable of additional lateral flexion to the right, but will not laterally flex to the left because of increased pain; once again this is because the synovial fold is entrapped on the left side and left lateral flexion increases meniscus compression, pain, and spasm. This is also why the patient is antalgic to the right; such positioning reduces left sided synovial fold compression, pain, and spasm.
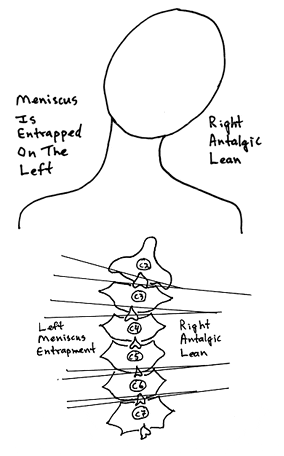
Additional clinical evaluation will reveal no signs of radiculopathy; no alterations of superficial sensation in a dermatomal pattern, and no signs of motor weakness or altered deep tendon reflexes. An important clinical feature is that although the patient will not laterally flex the cervical spine to the left because of increased pain and spasm, left cervical lateral flexion against resistance without motion (the doctor holds the patient’s head so that there is no motion even though the left-sided cervical muscles are contracting) will not increase the patient’s pain. This is because the involvement is not muscular. Muscle contraction against resistance will not increase pain as long as the joint does not move in the meniscoid block syndrome.
A typical treatment protocol to manage the synovial fold entrapment syndrome is that the patient is manipulated in an effort to free the entrapped meniscus. The most successful manipulation would induce additional right lateral flexion; in other words, the manipulation would cause further right side antalgia. Such a maneuver would cause both a gapping of the facets on the left side as well as a tensioning of the left side facet capsules, together pulling free the entrapped synovial fold.
When the precise level of synovial fold entrapment is ascertained and that precise level is manipulated in the appropriate direction to cause the intended neurobiomechanical changes, it is referred to by chiropractors as a “spinal adjustment.” The depth and speed of such an adjustment must be sufficient to overcome local muscle spasms that reflexively exist as a consequence of the pain the patient is experiencing. Following this first manipulation/adjustment, the patient may benefit from 10-15 minutes of axial traction to the cervical spine. Experience suggests that most patients will benefit from the application of a soft cervical collar, worn continuously until the following day.
The patient is evaluated and manipulated/adjusted again the second day, followed once again by optional axial cervical traction, but there is no need for the soft cervical collar on the second day. The patient is given the third day off, returning the fourth day for a final evaluation and adjustment/manipulation. It is typical for complete symptomatic resolution to occur in a period of 3 – 5 days following onset and treatment.
An important caution in adjusting/manipulating the meniscoid block lesion is to not do so in such a manner that it straightens the right antalgic lean. Recall that the patient is antalgic to the right because the synovial fold is entrapped on the left side. To attempt to straighten the right antalgic lean out will increase the meniscoid compression, pain and spasm, making the patient truly unhappy. In contrast, the adjustment/manipulation should be made in such a manner that the right antalgic lean is enhanced, gapping the left sided articulations, freeing the entrapped synovial fold, reducing pain and spasm.
As described in the eighth edition of his book (1982) Textbook of Orthopaedic Medicine (9), orthopaedic surgeon Sir James Cyriax describes how the fibers of the multifidus muscles blend with the facet joint capsular fibers. Chiropractic orthopedic training indicates that at the beginning of any joint movement, appropriate local articular proprioception will quickly initiate a contraction of the multifidus muscle, tightening the capsular ligaments, and pulling the meniscus of that joint into such a position that it cannot become entrapped. This suggests that the etiology of the meniscoid block syndrome is a failure of appropriate proprioceptive driven reflexes, indicative of a long-standing biomechanical problem. It is reasonable and appropriate to treat the long-standing biomechanical problem with a more prolonged series of spinal adjustments/manipulations and indicated rehabilitation. Failure to do so often results in frequent reoccurrences of the synovial fold entrapment syndrome following trivial mechanical environmental stresses.
[wc_fa icon=”ellipsis-h” margin_left=”” margin_right=””][/wc_fa]
SUMMARY
INTERPRETATION
If a patient’s antalgic lean is to the right, the positioning reduces pressure on the left sided facet injury and therefore has Left-sided synovial joint entrapment. In contrast, any left lateral flexion increases the pinch and associated pain on the entrapped synovial fold. The cervical muscles are in spasm as a consequence of the antalgia and pain.
TREATMENT
The only solution for this problem is to manually adjust the right cervical spine in lateral flexion at the C4-C5 articulation level. This adjustment is designed to make the antalgic lean worse; remember, the patient could slightly laterally flex the cervical spine to the right without aggravating the condition.
If an adjustment has enough velocity and depth to overcome the resistance of the increased tone from the spasmed musculature, that movement could be successful, it would gap the left sided C4-C5 facetal articulation, freeing the entrapped synovial fold. If successful, the patient should notice 50-80% improvement in antalgia, pain, and motion, essentially instantaneously.
FOLLOW-UP
The patient should be adjusted in a similar fashion the very next day, as noted above. Typically, there is no adjustment the third day, but the patient is once again adjusted the fourth day. Residual muscle hypertonicity and joint stiffness should be resolved within 3-5 days.
[wc_fa icon=”ellipsis-h” margin_left=”” margin_right=””][/wc_fa]
The Personal Injury Institute – Personal Injury Report is a monthly publication by me, Dr. Matthew J. DeGaetano, DC, Certified in Whiplash and Brain Traumatology and Colossus. I am a 1997 graduate of Parker College of Chiropractic. I have managed about 6,000 whiplash injury cases in NY, Texas, and New Mexico in the past 17 years. I am the personal consultant for over 400 offices and over 300 personal injury law firms nationally.
The purpose of The Personal Injury Institute – Personal Injury Report is to keep you updated on relevant academic concepts pertaining to whiplash injury patients. I hope that the information is useful in terms of enhanced understanding, as well as helpful for the personal injury attorneys to deal with insurance claim adjusters, dealing with Colossus systems and adverse medical experts.
Our clinics are well informed and trained in these concepts of personal injury and the details of Colossus and will be a valuable asset in personal injury cases, in terms of both academics and treatment. Additionally, expert chiropractors and your law firm will have access to daily phone consultation with me, to discuss any pertinent issues faced by them, on a particular case.
I hope that you find this Report as a valuable resource.
Sincerely,
Matthew J. DeGaetano, DC
References
1) Cox MW, McCarthy M, Lemmon G, Wenker J. Cervical spine instability: clearance using dynamic fluoroscopy. Current Surgery.January 2001;58(1):96-100.
2) Pearson AM, Ivancic PC, Ito S, Panjabi MM. Facet joint kinematics and injury mechanisms during simulated whiplash. Spine (Phila Pa 1976). 2004 Feb 15;29(4):390
3) Panjabi MM, Ito S, Pearson AM, Ivancic PC. Injury mechanisms of the cervical intervertebral disc during simulated whiplash. Spine (Phila Pa 1976). 2004 Jun 1;29(11):1217-25.
4) White AA 3rd, Johnson RM, Panjabi MM, Southwick WO.Biomechanical analysis of clinical stability in the cervical spine. Clin Orthop Relat Res. 1975;(109):85-96.
5) Barnsley L, Lord SM, Wallis BJ, Bogduk N. The prevalence of chronic cervical zygapophyseal joint pain after whiplash. Spine. 1995; 20:20-5.
6) Lord SM, Barnsley L, Wallis BJ, Bogduk N. Chronic cervical zygapophyseal joint pain after whiplash. A placebo-controlled prevalence study. Spine. 1996; 21: 1737-1745.
7) Macnab I. Acceleration extension injuries of the cervical spine. In Rothman RH, Simeone FA (eds): The Spine, ed 2. Philadelphia, WB Saunders. 1982; Vol. 2: p.648.
8) Foreman SM, Croft AC. Whiplash Injuries. Baltimore: Williams and Wilkins, 1988, p.323.
9) Mendelson G. Not “cured by a verdict.” Effect of legal settlement on compensation claimants. Med J Aust. 1982; 2: 132-4.
10) Mendelson G. Follow-up studies of personal injury litigants. Int J Law Psychiatry. 1984; 7: 179-88.
11) Barnsley L, Lord SM, Bogduk N. Whiplash injury. Pain. 1994; 58:283-307.
12) Kaneoka K, Ono K, Inami S, Hayashi K. Motion analysis of cervical vertebrae during whiplash loading. Spine. 1999. Vol. 24: 763-770.
13) Giles LGF, Harvey AR. Immunohistochemical demonstration of nociceptors in the capsule and synovial folds of human zygapophyseal joints. Br J of Rheumatol. 1987; 26: 362-364.
14) Bogduk N, Jull G. The theoretical pathology of acute locked back: a basis for manipulative therapy. Man Med. 1985; 1:78-82.
15) Giles LGF. Pathoanatomic studies and clinical significance of lumbosacral zygapophyseal (facet) joints. JMPT. 1992: 15:36-40. 2. Webb AL, Collins P, Rassoulian H, Mitchell BS; Synovial folds – A pain in the neck?; Manual Therapy; April 2011; Vol. 16; No. 2; pp. 118-124.
16) Junghanns H; Schmorl’s and Junghanns’ The Human Spine in Health and Disease; Grune & Stratton; 1971.
17) Idczak GD; Aspects of Manipulative Therapy; Churchill Livingstone; 1985.
18) Grieve G; Modern Manual Therapy of the Vertebral Column; Churchill Livingstone; 1986.
19) Grant R; Physical Therapy of the Cervical and Thoracic Spine, second edition; Churchill Livingstone, 1994.
20) Cailliet R; The Illustrated Guide to Functional Anatomy of the Musculoskeletal System, American Medical Association, 2004.
21) Bogduk N; Clinical Anatomy of the Lumbar Spine and Sacrum, fourth edition; Elsevier, 2005.
22) Friedrich KM. MD, Trattnig S, Millington SA, Friedrich M, Groschmidt K, Pretterklieber ML; High-Field Magnetic Resonance Imaging of Meniscoids in the Zygapophyseal Joints of the Human Cervical Spine; Spine; January 15, 2007, Volume 32(2), January 15, 2007, pp. 244-248.
23) Cyriax J; Textbook of Orthopaedic Medicine, Diagnosis of Soft Tissue Lesions, eighth edition; Bailliere Tindall, 1982.
